
Do I Have OCD?
Rather than starting with the definition of OCD, it’s more helpful to describe the lived experience first. Life with OCD can be extremely challenging. Constant intrusive thoughts and repetitive behaviours can interrupt everyday routines, and the nature of these thoughts often makes it difficult to reach out for help.
Many people do not tell their doctor the full extent of what they are experiencing because they are afraid of being judged or misunderstood.
Because of this, some people with OCD are initially diagnosed with anxiety rather than OCD and may be prescribed antidepressants or other medications at a lower dose, and may not receive a referral for appropriate therapies.
Quick Links
- Do I Have OCD?
- Can you have OCD without Obsessive Cleaning?
- What is OCD?
- What Are The Symptoms of OCD?
- Common Obsessions
- Common Compulsions
- The OCD Cycle vs The OCD Spiral
- How OCD Affects The Nervous System
- Is OCD Connected to CPTSD Or Trauma?
- How OCD Affects Relationships and Daily Life
- Can I Recover From OCD?
- Final Thoughts
Can You Have OCD Without Obsessively Cleaning?
Social media and films have led many of us to believe that people with OCD obsessively clean their houses. Friends will refer to each other as “a bit OCD” and laugh about how tidy their houses are. This is incredibly misleading, because not everyone with OCD is obsessed with cleanliness. It also creates a situation where people will rule out OCD as a problem because they don’t fit the popular caricature.
However, a large cohort of OCDers do spend a few hours a day cleaning their houses and not all of them do it because they are bothered by germs. Some do it because they feel the urge to get up and do something.
Don’t be put off getting a diagnosis if your house isn’t dust free because the media can’t diagnose you, only your doctor can do that.
What is OCD?
Obsessive Compulsive Disorder (OCD) is a mental health condition where intrusive thoughts trigger compulsions that a person feels driven to repeat in order to reduce anxiety.
OCD often begins during the teenage years, when life already feels confusing and overwhelming. It is also commonly seen alongside neurodivergent conditions such as autism and ADHD. The symptoms of OCD are usually divided into two categories: obsessions and compulsions.
Obsessions are intrusive thoughts, images, or urges that appear suddenly and cause distress. For example, someone might experience unwanted urges to do something they would never actually want to do, or vivid “what if” scenarios that play out like short films of something terrible happening.
Compulsions are behaviours or mental rituals that a person feels driven to perform in order to reduce anxiety or prevent something bad from happening. These might include washing hands repeatedly, tidying or arranging objects for long periods of time, checking things over and over again, counting, or repeating certain words or prayers.
Importantly, people with OCD usually recognise that these thoughts are not rational and do not reflect who they really are. Many feel frustrated or ashamed of the thoughts they experience. If this sounds familiar, it’s important to know that you are not alone, and none of this is your fault. I’ll explain more about why these thoughts happen later in the article.
What Are The Symptoms of OCD?
The symptoms of OCD usually fall into two groups. Some happen inside your mind, known as obsessions, and others involve actions you feel compelled to carry out, known as compulsions.
Obsessions are intrusive thoughts, images, or worries that keep returning even when you try to ignore them. Compulsions are behaviours or mental rituals that people feel driven to perform in an attempt to reduce the anxiety those thoughts create.
It is also possible to experience what psychiatrists sometimes refer to as “Pure O” OCD, where the compulsions are not obvious physical behaviours. Instead they happen internally, such as repeating phrases in your mind, mentally checking things, or analysing thoughts over and over.
Because of this, some people only recognise the obsessive side of the condition. If you identify with the intrusive thoughts but not the visible compulsions, that does not mean OCD cannot apply to you.

Common Obsessions (Intrusive Thoughts)
- Fear of harming someone, even though you have no desire to do so
- Fear of contamination or illness
- Persistent doubts about whether you have done something wrong
- Intrusive sexual or violent thoughts that feel disturbing or shameful
- Fear of making a mistake that will lead to something terrible happening
- Constant worry about morality, religion, or being a “bad person”
- Safety anxiety, such as whether doors are locked or appliances are off
- A strong feeling that nothing’s ever “just right”
- Distressing images or videos that replay in your mind
- Fear that something bad may happen
These thoughts are usually unwanted and distressing. People with OCD often recognise that the thoughts don’t reflect who they really are, but it’s hard to ignore and separate yourself from something that’s going on in your own brain.
Common Compulsions (Actions or Mental Rituals)
- Repeated checking of locks, appliances, or other safety concerns
- Excessive cleaning, washing, or disinfecting things that you touch
- Excessive washing of hands causing dry skin and irritation
- Arranging objects until they feel symmetrical or “just right”
- Repeatedly asking others for reassurance
- Avoiding certain places, objects, or situations that trigger anxiety
- Repeating phrases, numbers, or prayers in your mind
- Counting behaviours such as steps, taps, or repetitions
- Touching objects in a specific order or pattern (especially light switches)
- Researching symptoms or information repeatedly to reassure yourself
Compulsions usually provide temporary relief from anxiety, but the relief rarely lasts. Over time the cycle of intrusive thoughts and compulsive behaviour can become exhausting and time-consuming.
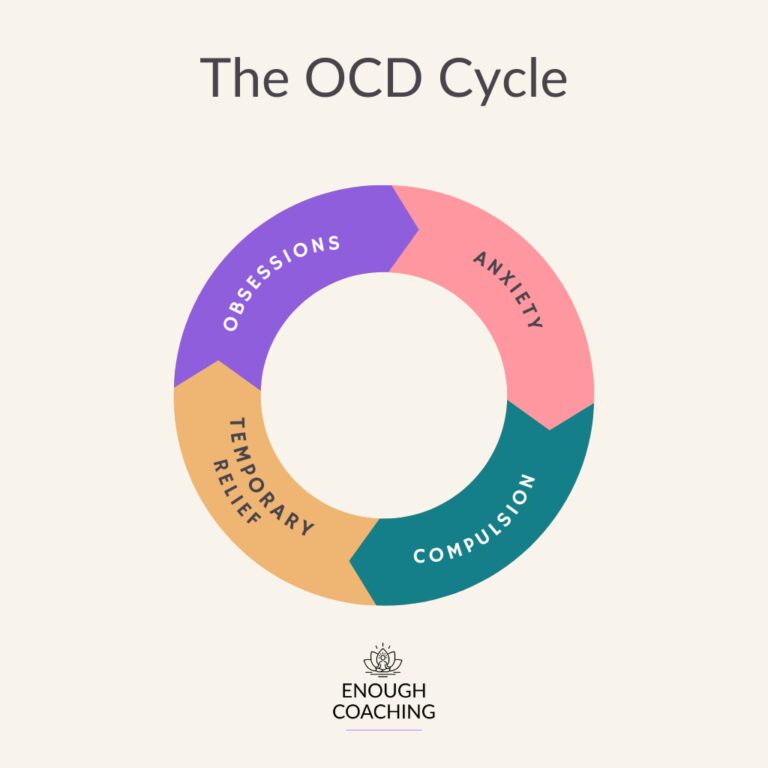
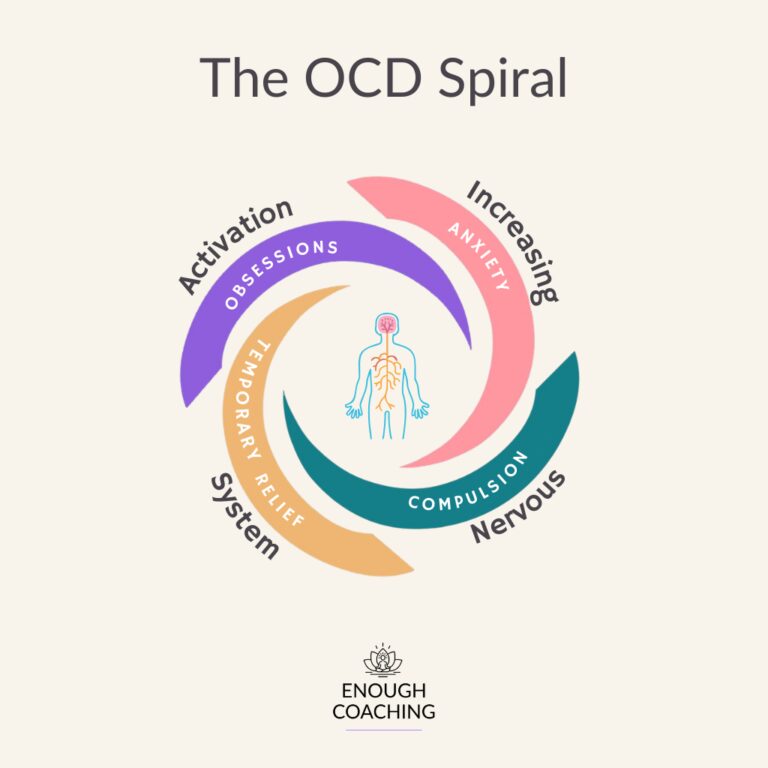
The OCD Cycle vs The OCD Spiral
OCD is often described in textbooks as a cycle, however from my personal experience and recovery I see it more as a Spiral. Each time a compulsion relieves anxiety, the brain mistakenly learns that the behaviour helped. This can make the urge to repeat the behaviour happen more frequently.
At the same time, the intensity of the experience is heavily influenced by stress levels and external triggers. When someone is already under pressure or feeling overwhelmed, the types of intrusive thoughts can be more intense.
Because of this, OCD tends to worsen during periods of high stress and become easier to manage when the nervous system is calmer.
How OCD Affects The Nervous System
The human nervous system is designed to protect us from threats in the outside world. Many years ago, if a human encountered a wild animal they needed a surge of adrenaline to defend themselves or hunt for dinner. That response helped our ancestors survive.
Today most of us are no longer facing predators in the wild. If we want to see a wild animal we usually have to go on safari or visit a zoo.
Unfortunately our primitive brain can’t tell the difference between what we actually see and what we visualise in our thoughts. When the mind perceives danger the
body can respond in the same way it would to a real physical threat.
This activates the fight or flight response, placing the nervous system into what is known as a sympathetic state. Our pupils dilate, heart rate increases, and digestion slows as the body prepares to deal with danger.
If the nervous system stays in this heightened state for long periods of time, the effects can spread throughout the body. Chronic stress can contribute to muscle tension, inflammation, disrupted sleep, and ongoing anxiety.
Over time, conditions like OCD can place a significant strain on the nervous system. Many people also experience exhaustion, sleep debt, and a weakened immune response when their body spends too long in a state of constant alert.
Is OCD Connected to CPTSD Or Trauma?
It’s true that many people receive diagnoses of both OCD and CPTSD. Both conditions have symptoms in common and some practitioners believe that OCD can sometimes be caused by traumatic experiences.
But it could also be genetic. Research indicates that between 10% and 20% of children with a parent who has OCD will develop OCD themselves.
A balanced view of this information is that it could be either genetic or environmental and that both conditions involve nervous system dysregulation and respond well to Exposure and Response Prevention and Cognitive Behavioural therapies.
How OCD Affects Relationships and Daily Life
OCD can affect many areas of daily life. It can create feelings of shame or self-judgement about the thoughts you experience, as well as the amount of time spent trying to find relief through behaviours such as cleaning, washing, counting, or checking.
You may find it difficult to talk honestly with your partner about what is happening in your mind, which can create a barrier to intimacy. At work, the condition can also make everyday tasks more difficult. You might be late for work because you had to drive home to check that the front door is locked or that the iron wasn’t left on. Perhaps you reread every email several times before sending it, trying to make sure the wording and tone are exactly right.
Over time these patterns can begin to affect confidence, relationships, and the ability to relax and enjoy life. Many people with OCD feel isolated, carrying the experience privately while the outside world is oblivious.
But it does not have to stay that way.
Can I Recover From OCD?
Yes, recovery from OCD is possible. The first step is to fully realise that your thoughts are not a reflection of your morality or principles. For many people, the shame surrounding these thoughts is what keeps them stuck in the OCD Spiral.
When you know, in your bones, that you wouldn’t ever follow through on any of those thoughts the self judgement and shame start to fade away.
The next step is to start reducing the compulsive rituals. Rather than trying to eliminate everything at once, it helps to approach this gradually. Begin with a few behaviours that feel easier to let go of so that you can build confidence.
As those fall away, you can begin working on the rituals that have the biggest impact on your daily life.
You can also support this process by learning ways to settle your nervous system. Practices such as meditation, gentle somatic exercises, or calm creative activities like painting, singing, or dancing can help shift your body out of a constant stress response. Anything that helps you reconnect with your body rather than staying trapped in your thoughts can be helpful.
Physical movement can be particularly powerful. When the body moves, it encourages neuroplasticity, the brain’s natural ability to form new patterns and pathways. As your nervous system becomes steadier, it becomes easier to notice the situations that trigger intrusive thoughts and compulsive behaviours.
Over time this interrupts the connection between your intrusive thoughts and your rituals and the spiral loses momentum. Instead of reacting automatically from anxiety, you begin to respond with more choice and control.
OCD and trauma often occur alongside each other and interact, so it can be helpful to work with someone who understands these patterns and can support you along the way.
My Story
The turning point for me came when I realised that the intrusive thoughts did not reflect my core values at all. For a long time I believed the thoughts meant something about who I was as a person. That belief created a huge amount of shame and self-judgement.
Once I understood that intrusive thoughts are simply thoughts, and not a reflection of my character, a lot of that shame began to fall away. The thoughts lost much of their power.
From there I began reducing the compulsive rituals, one at a time. I started with a few small behaviours that felt easier to let go of so that I could build some confidence. As those fell away, I worked on the rituals that were having the biggest impact on my daily life.
Over time the spiral started to slow down. The thoughts appeared less often, and when they did appear I started to joke that they were like a dodgy car alarm in my head.
Interestingly, I chose to keep a couple of harmless habits, like folding crisp packets neatly into triangles. They don’t affect my life in any meaningful way, and keeping them acted as a reminder of how far I’d come.
Over the course of a couple of years I went from experiencing ten intrusive thoughts or mental “videos” a day to perhaps one or two a year. When they do appear now, I recognise them immediately for what they are and swipe them away like an unwanted notification on my phone.
Final Thoughts
If you recognised yourself in parts of this article, you’re not alone. Many people live with intrusive thoughts and compulsive behaviours for years before they reach out for help.
OCD can feel confusing and isolating, particularly because the intrusive thoughts clash with your values or sense of who you are. It is important to remember that these thoughts are not a reflection of your character – you are not your thoughts. They are simply a pattern that the mind and nervous system have become stuck within.
With understanding, patience, and the right support, it is possible to move beyond the OCD Spiral. Recovery rarely happens all at once, but small steps taken consistently can gradually reduce those intrusive thoughts and give you hours back in your day.
